“MEET THE MONSTER” – FACTS ABOUT DIPG
Diffuse Intrinsic Pontine Gliomas (DIPG) are rare and highly aggressive brain tumors found in the pons which is located at the base of the brain. The pons controls many of the body’s most vital functions such as breathing, blood pressure and heart rate . DIPG is a kind of glioma, meaning that it originates from the “glial cells” (connective/supporting) of the brain. Gliomas of the brainstem are uncommon in adults, but in children they are the leading cause of deaths from brain tumors. Typically, children with a DIPG are diagnosed between the ages of 5 and 9. The tumors occur equally in boys and girls. DIPGs makes up 10-15% of all brain tumors in children, with about 100-300 new cases diagnosed each year in the United States. Unfortunately, the prognosis for children with a DIPG remains poor. The median survival time following diagnosis – with treatment – is 9 to 12 months (with less than a 10% survival rate after two years and less than 1% after five years).
. DIPG is a kind of glioma, meaning that it originates from the “glial cells” (connective/supporting) of the brain. Gliomas of the brainstem are uncommon in adults, but in children they are the leading cause of deaths from brain tumors. Typically, children with a DIPG are diagnosed between the ages of 5 and 9. The tumors occur equally in boys and girls. DIPGs makes up 10-15% of all brain tumors in children, with about 100-300 new cases diagnosed each year in the United States. Unfortunately, the prognosis for children with a DIPG remains poor. The median survival time following diagnosis – with treatment – is 9 to 12 months (with less than a 10% survival rate after two years and less than 1% after five years).
SYMPTOMS:
Since DIPGs often affect the cranial nerves, many of the early symptoms of a DIPG appear in the facial muscles, often affecting the eye and eyelid movements. However, the tumor grows so fast that other symptoms often appear suddenly and worsen quickly. The most common symptoms of DIPG are: • Problems with eye movement; • Facial weakness – drooping on one side of the face; • Sudden appearance of hearing problems; • Trouble chewing or swallowing; • Limb weakness, difficulty standing or walking, abnormal gaits, clumsiness, unbalanced limb movements; • Headache; and, • Nausea and vomiting from brain edema (swelling) or hydrocephalus.
HOW IS A DIPG DIAGNOSED?
DIPGs are most commonly diagnosed from imaging studies, including Computerized Tomography scans (CT scan), Magnetic Resonance Imaging (MRI – most common) or Magnetic Resonance Spectroscopy (MRS).
A CT scan is a diagnostic imaging procedure that uses a combination of x-rays 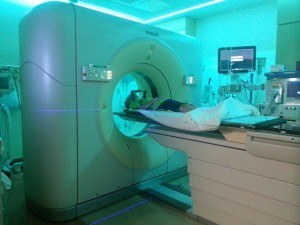 and computer technology to produce cross-sectional images of the body. CT scans are more detailed than general x-rays.
and computer technology to produce cross-sectional images of the body. CT scans are more detailed than general x-rays.
An MRI is a diagnostic procedure that uses a combination of large magnets, radio frequencies and computer technology to produce detailed images of organs and structures within the body. MRIs provide greater anatomical detail than that of a CT scan and do a better job of distinguishing between tumors, tumor-related swelling and normal tissue.
MRS is a diagnostic study that is conducted during an MRI to detect the presence of certain organic compounds around the tumor tissue that can identify the tissue as normal or tumor.
TREATMENT OPTIONS:
Surgery: Surgery is not an option for children with a DIPG because the tumor infiltrates extensively into normal brain tissue, making surgical removal impossible. There is no way to avoid cutting out healthy brain tissue which is vital for survival.
Radiation Therapy: Radiation therapy is the primary treatment for DIPG and is the current Standard of Care. It uses high-energy rays (radiation) from a specialized machine to focus in on the tumor area and damage or kill cancer cells and shrink tumors. Radiation therapy typically lasts 6 to 7 weeks with treatments administered over a course of approximately 30 days. Conventional limited-field radiation produces responses in 75-90 percent of children with DIPGs. If symptoms are present at diagnosis, this therapy can sometime improve how the child feels. However, these responses are short-lived, lasting about six to nine months on average before the tumor starts to regrow and the symptoms reappear.
Experimental Chemotherapy: To date, chemotherapy has not proven effective against DIPG. According to Dr. Michelle Monje, Assistant Professor of Neurology at Stanford, “there have been over 200 clinical trials of chemotherapy drugs for DIPG, and none have shown any survival benefit.” The main reason for this is likely because most chemotherapy agents are not able to get into the tumor at all because of the high pressure inside the pons and the blood-brain barrier (a filtering mechanism of the capillaries that carries blood to the brain and spinal cord tissue, blocking the passage of certain substances). To try to get around this problem, researchers are studying different agents that may be able to pass through the blood-brain barrier as well as other new and innovative ways to get drugs directly into the tumor (including Convection Enhanced Delivery – CED). Work to discover new and effective agents also continues.
PARENT TIP: “While most of your focus is on your child during this time, be sure to take care of yourself as well. Keep in mind that many chemotherapy treatments will compromise your child’s immune system so if you become sick, you may put your child at risk for additional complications.”
Biopsy: Although it is not possible to remove the entire tumor surgically, recent clinical trials and studies have shown that it is generally safe to perform a biopsy of the tumor (remove small amounts of tumor tissue for diagnostic testing). The two primary purposes for performing a biopsy are: (1) to confirm the diagnosis, and (2) for research and to obtain a better understanding of the genetic make-up of the individual tumor – for potential future individualized treatment. As one example of this, in a current clinical trial being performed by the Dana-Farber Cancer Institute, titled “Molecularly Determined Treatment of Diffuse Intrinsic Pontine Gliomas (DIPG),” patients diagnosed with a DIPG undergo a biopsy shortly after diagnosis. Then, based on the genetic make-up of the tumor researchers have learned from the biopsy (typically several weeks later), the patient goes on to receive one or more chemotherapy drugs thought to be specifically tailored to target the specific “mutations” identified. Since it is now known and generally accepted that all DIPGs are not genetically identical, the benefits of this individualized treatment approach are obvious (and include ruling out other drugs and clinical trials which may not apply). However, the benefits must be weighed against the risks associated with undergoing the biopsy procedure – which is still a complicated brain surgery involving a several day hospitalization.
PARENT TIP: “Before making a decision on any treatment, consider writing down all of the pros and cons of the proposed treatment, what information about your child’s condition was known at the time, and ultimately, why the treatment selected (if any) was chosen. Hindsight always seems to be 20-20. Having this information in writing can be a helpful reminder of why the decision was made – when it was made – if circumstances change down the road.”
SOURCES:
1. Dana-Farber Cancer Institute
2. DIPG Registry
3. Weill Cornell Brain and Spine Center
4. National Institutes of Health (NIH)
5. Stanford Medicine News Center (May 4, 2015)
6. Clinical Trial – Molecularly Determined Treatment of Diffuse Intrinsic Pontine Gliomas (DIPG)
Research and recent advancements
January 2015 – Overturning Dogma to Open the Black Box of DIPG
May 2015 – Existing Drug May Treat the Deadliest Childhood Brain Tumor
April 2018 – Altered Immune Cells Clear Childhood Brain Tumor in Mice
OPEN/RECRUITING DIPG CLINICAL TRIALS A full list of all open and recruiting clinical trials for DIPG can be found here or at www.clinicaltrials.gov.

